 Common names for Patellofemoral Pain Syndrome (PFPS) are Chondromalacia patella, anterior knee pain, runners knee, patellofemoral tracking disorder.
Common names for Patellofemoral Pain Syndrome (PFPS) are Chondromalacia patella, anterior knee pain, runners knee, patellofemoral tracking disorder.
What is Patellofemoral Pain?
![]() Patellofemoral pain is felt at the front of the knee and typically comes on gradually typically comes on gradually.
Patellofemoral pain is felt at the front of the knee and typically comes on gradually typically comes on gradually.
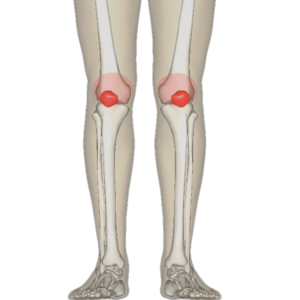
Normally the patella (your knee cap) glides in a groove in your femur when bending your knee.
It is believed PFPS results from abnormal Patella tracking (not gliding smoothly in the groove) causing excessive compression on the under surface.
What Causes Patellofemoral Pain?
- Quadriceps weakness (particularly poor activation of your VMO/inside quads) causing an imbalance.
- Excessive knee soft tissue tightness
- Tight Quads and Iliotibial band
- An increased quadriceps angle (Q-angle)
- Hip weakness (particularly Hip abductors and external rotators)
- Altered foot biomechanics eg. over-pronation
Generally, there is always a combination of these factors causing a significant imbalance of forces on the knee cap, leading it to be pulled to one side (like a tug of war!). It is generally pulled laterally.
Symptoms and Signs
- Anterior knee pain
- Knee stiffness with prolonged knee flexion eg. sitting in movie or driving.
- Activity-related pain: Running, squatting, stair climbing (especially going down), kneeling, cycling, swimming breaststroke.
- Tenderness/pain on compression if the knee cap
- Crepitations or Grating sensation
- Giving way
- Swelling around the knee cap
Risk Factors:
- Female gender
- Iliotibial band syndrome (ITB syndrome)
- Training: Long distance running, training on hard surfaces, hills, stairs
Note: it is important to remember that muscle dysfunction and repetitive loading of the Patellofemoral joint rather than fixed biomechanical factors and the major contributors to PFPS(Baker and Juhn 2000) and so there is a lot that can be done to help.
Prognosis
Depends on co-existing conditions, but poor if causative/aggravating factors and not addressed. If symptoms have been there for over 12 months you will have a poorer prognosis but do lose heart, it can get a lot better, you just need to persevere and stick at it 🙂
Test yourself! To see how stable your hips are.
Self Treatment Exercises
1. Single Leg Bridges

Tip: alternate legs and switch your core on.
2. Decline Mini Squats

Action: Do not push into pain (if it is sore, don’t go as low), you do not need to go below parallel. Squat like you are going to sit down in a chair and do not let your knees go past your toes.
Perform 3 sets of 12, nice, slow and controlled.
Tip: look up to the top of the wall to help your balance.
3. Foam Roller:

Roll all the way from the knee to the hip, making sure you do it slowly.
Spend 2 minutes on the side as shown and then 2 minutes on the front/quads.
Tip: try to keep your feet off the ground and DO NOT LET PAIN PUT YOU OFF, it will get easier.
4. Clams:
Lying on your side as shown. keeping your ankles together, lift your top knee 20cm, then lower down again (don’t drop it!)
Goal = 1 set of 50, if you are doing them right, you will need to build up to this.
Tip: Keep your top elbow down on the ground and hips rolled forward.
 5. Quads stretch:
5. Quads stretch:
Hold this stretch for 1 minute.
You may need to put a cushion or towel under the planted knee!
Tip: you do not need to lunge forward, to add more stretch, tuck your bum in under you or put back foot up on something (eg. wall or foam roller).
Note: if this hurts the knee (even with padding) then stop doing it and wait a couple of weeks before building it in.
Do these exercises two times daily.
What Else Helps
- Brace: while rehabbing your knee, a brace can help keep you moving, such as a Patella Tracker
- Orthotics: the use of Orthotics reduces PFPS in the short to medium term and addresses bio-mechanic deficiencies on the foot.
- Ice: after exercise, after a long day or when there is any pain ice minutes for 10 -15 at a time (no longer).
- Rest, give it a couple of weeks rest. this gives you a great time to get a head start on the exercises and really start the rehab off well.
- Altering training: shorter distance, get off hard surfaces, cross-train.
- Footwear: throw out old shoes, stay away from shoes with poor support eg: Flip-Flops, jandals, sandals, slippers.
Often it is not the knees fault all this pain and discomfort happens, so to treat this condition it is important to look above (quads, ITB, hip) and below (foot, calf).
Follow this advice for at least 12 weeks (yes three months, you NEED to be serious about this to decrease the risk of early knee arthritis and ongoing pain.)
Chondromalacia Patella is NOT PFPS
Chondromalacia Patella is commonly over diagnosed and is when the articular cartilage on the undersurface of your knee cap is damaged.
The prevalence of this is far less than Patellofemoral pain syndrome but generally occurs if PFPS is left too long as the cartilage gradually softens and degenerates.
This can be confirmed with an MRI. The rehab exercises and advice for Patellofemoral pain mentioned above WILL HELP this also, it will just be a longer recovery period.
If you have any questions feel free to comment below.
Please share, comment, follow and let me know how you get on!
You may also like:
Glute activation, the missing link
Quick stability and balance test
A good research paper if you want more info on PFPS research




Hi there and thank you so much for this resource! I’ve been struggling with PFPS on and off, unable to do sports for about 8 months now and was getting a bit discouraged… but now I’m excited and hopeful for recovery again! I was just wondering, would you recommend doing any low resistance cycling on top of this at all? And what is your opinion on McConnell taping? Thank you!
Hi Charlotte
Good on you, there is a lot you can do to help it so never get discouraged! Yes, you can do some cycling on top of that but try every second day, not days in a row.
Yes, I use the medial glide McConnell taping with PFPS a lot with great results so if it works for you, utilize it while you rehab.
Best of luck!
Shaun
Hi Charlotte, did you have any luck with this?
I’ve got symptoms of knee aching like hell when in a bent position. Been trying to find a decent program to help me get back to full fitness!