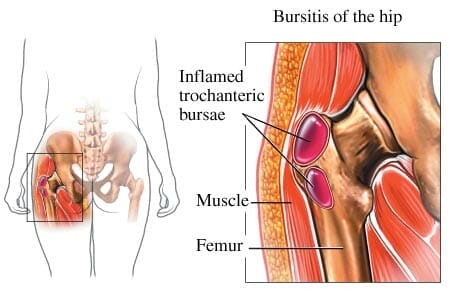
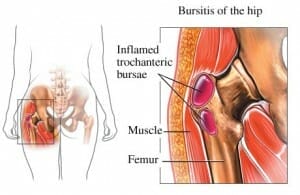
Trochanteric bursitis is an all too common cause of hip pain throughout the population, from athletes to the elderly.
In this post I will clearly explain, what trochanteric bursitis is, what causes it, and what the best rehabilitation exercises and self-treatment techniques that can be done at home to help you get back to your best!
Also often called: Greater trochanteric bursitis, trochanteric pain syndrome
Where is the Bursa and What Does it Do:
All bursa in your body (there are about 160 of them!) work to help all the structures in your body move smoothly.
The bursa is like a small balloon of fluid – normally a very thinly filled one – and in this case it lies over the greater trochanter so your iliotibial band (as seen in the picture to the right) can glide over the bone smoothly.
What is the cause of trochanteric bursitis?
The two main causes are:
- The most common cause is repetitive friction or compression of the bursa by the structures/tissue that glide over it.
This is what I am going to tell you about in more detail below as there are some main contributing factors that lead to the excessive friction and compression on the bursa which have to be addressed to get long term results.
- The other is direct trauma such as a fall on to you hip.
Both of these cause the inflammation within the bursa so that if is blown up by the inflammatory fluid like a balloon and the walls of the bursa thicken.
Contributing factors (lets find the real reason you get bursitis!):
The simple mechanism of injury in cases without direct trauma is excessive friction/compression of overlying tissues on the trochanteric bursa.
What leads to this excessive friction/compression is the important thing – if we find this, we can treat this very well!
- Osteoarthritis – of the hip or low back
- Tightness of the ITB – The iliotibial band crosses over the bursa, so if this is tight it will cause excessive compression and friction.
- Leg length discrepancy – Causing a muscle imbalance and glute dysfunction in the pelvis.
- Weak hip abductors (glutes medius and gluteus minimus) – These are the muscles that stop your leg going inwards while walking and stop your hip dropping – so if these are weak you will have poor hip stability and biomechanics – putting more pressure on the bursa.
- Weak core
- Tight or over active and tensor fascia latae – This muscle attaches on to the iliotibial band and so if this is working too hard (such as when your hip abductors are weak) it causes tension on the ITB.
- Risk factors
- Higher prevalence in women than men; 4 times more likely! This is due to decreased oestrogen post-menopause decreasing muscle tone and also broader hips and a narrow stance in women.
How Do You Know if it is Trochanteric Bursitis?
Presentation/signs and symptoms
The main complaint is aching in the upper lateral(outside) thigh.
If acute/quick onset, pain can be sharp and intense. However, pain in chronic hip bursitis is usually dull and diffuse and may radiate down to or below the knee, mimicking low back radicular symptoms.
There is tenderness with direct pressure, such as when lying on the affected hip. Pain can disturb sleep and general mobility(walking).
Painful activities include prolonged standing, squatting, and the first steps after rising from a chair. Pain increases with hip flexion and external rotation. As in crossing affected leg over the other while sitting.
The main and most accurate test during physical exam is intense or sharp tenderness on deep palpation of the greater trochanter.
Lateral Hip Pain

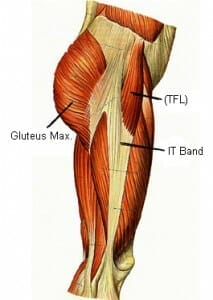
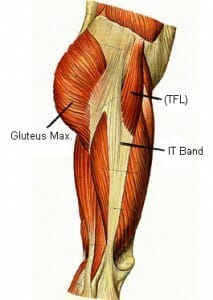
The primary (most common) cause of lateral hip pain is tendinopathy or dysfunction of the Gluteus Medius and Gluteus Minimus muscles(you can see in the image to the right that they attach straight onto the Greater Trochanter).
In a new study where over 800 patients with trochanteric pain syndrome were scanned, 50% had gluteal tendinopathy and just 20% had trochanteric bursitis.
So given that often gluteal tendinopathy is the primary cause of lateral hip pain it is important for long-term pain relief, rehabilitation exercises and correction of any biomechanical deficiencies (muscle imbalance, leg length discrepancy, poor foot mechanics etc) are followed through with and addressed.
Rehabilitation Exercises and Self-Treatment
1. Glute Strengthening:
Side lying hip abduction: Making sure to keep your top elbow down to stop your hips rolling back.
- 3 sets of 12 repetitions
Clams: Top elbow down again, keep your ankles together, lift the top knee up about 20cm.
- If you find it is too easy, roll your pelvis forward more.
- If it hurts your hip then place a towel or small pillow between your knees
- Your Goal is 50 repetitions, nice and slow
2. Advanced hip strengthening:
This is for really getting the hips strong and balanced out and best to start when you are recovering well and pain free.
Bulgarian split squat: Don’t get scared off by the name – you can do this! Just remember the back leg is just for balance – not to help you up and down.
- Tips: Make the front leg work. Start a good distance out from the step/chair. Take it slowly and control it.
- 3 sets of 8 repetitions.
3. Myofascial Release of Your Tight TFL (Tensor Fascia Latae muscle)

The TFL is, as you can see the image below a little muscle at the side of your hip. to find it, place your fingers on your ASIS which are the bones on either side of your pelvis at the front.
From the side of these, drop down a couple of inches and you should be right on it!
Lie on your side and place a ball under your TFL – you can use any ball you like, massage ball, lacrosse ball, tennis or golf ball.
Then slowly roll the ball around that area, working out all the knots and tight spots – this can take 2-5 minutes but is well worth your time!
And remember, a bit of trigger point pain is expected here.
- You can also check out this mobility WOD video – The main bit I want you to do is the ball work from about 3 mins and 36 seconds. This is a great release to do and will give your awesome relief!
4. Footwear:
Supportive footwear with arch and heel support is a huge plus as it stops your foot over pronating or supinating.
Over Pronating or Supinatinvg would put your hip in a bad position (try standing in bare feet and rolling your feet in and out and notice what it does to your hip position).
Alternatively you can go to the podiatrist and see if you need orthotics.
Maintenance and prevention – This is big, you cannot stop the exercises once the pain has gone – you can do them less, absolutely, but you need to persevere.
Should You Take Cortisone Injections
If you get one for your bursitis, remember it takes away the inflammation but it does not fix out the things that caused it such as hip stability. There is a high chance it will come back if you don’t rehab it.
Also it is important to get a clear diagnosis before injection as cortisone is basically poison for tendons (and remember only 20% of lateral hip pain is actually Bursitis – a lot more are tendinopathies).
Back pain?
Low Back Pain and dysfunction can have a big impact and even cause lateral hip pain so make sure you address this also.
Finally, check out this quick hip stability and balance test!